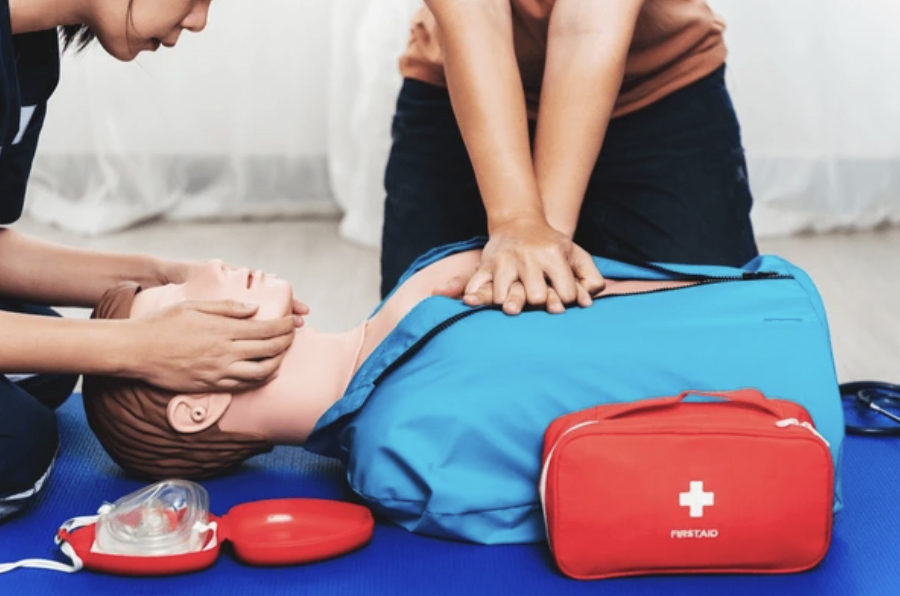
COVID-19 and the Risk of Sudden Cardiac Arrest
The damaging effects of COVID-19 are not restricted to the lungs. New information indicates that both the virus, and the drugs used to treat the infection, can affect cardiac health. When SARS-CoV-2, the virus that causes COVID-19, emerged in December of 2019, critical lung failure resulting from severe pneumonia was the primary concern. Increasing, data shows that other organ systems, including the cardiovascular system, are at risk. A retrospective study of 416 patients in Wuhan, China found that 1 in 5 confirmed COVID-19 patients developed cardiac injury. This observed harm to heart was associated with greater mortality. COVID-19 patients are developing heart problems – and are also dying of cardiac arrest.

The effects of COVID-19 on the heart
The precise mechanism by which SARS-CoV-2 causes cardiac damage is unknown. Additionally, speculation remains whether these emerging heart problems are caused directly by the virus or are a byproduct of severe illness. Acute respiratory distress, and the resulting oxygen deprivation, can cause damage throughout the body, including cardiac tissue.
Moreover, inflammation can make arterial plaque unstable, causing heart attacks. Alongside these byproducts of infection, there is also evidence suggesting that the virus damages the heart directly. Initial research indicates that SARS-CoV-2 infects lung cells by attaching to a receptor that is also present in heart tissue.
Regardless of the mechanism, the cardiac damage resulting from COVID-19 appears to profoundly affect a patient’s chances of survival. Researchers in Wuhan, China found that 51% of patients with cardiac injury died compared to 4.5% without. Early studies also indicate that everyone, not just those with pre-existing heart problems, are at risk of COVID-19-induced cardiac damage. Although this novel coronavirus may harm the heart in the absence of respiratory distress, the combination of acute lung infection and cardiac damage is particularly dangerous.
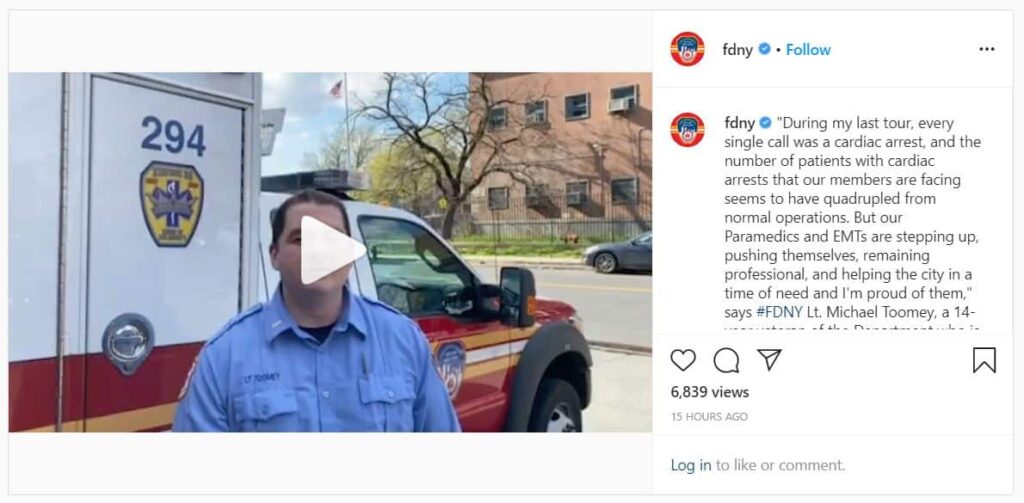
Cities are beginning to see the devastating impact that COVID-19 is having on people’s hearts. In New York City, the number of calls to EMS for cardiac arrest patients has skyrocketed. From March 30 to April 5, 2019, there were, on average, 69 cardiac calls daily, and 38% of those patients died. During the same period this year, there were, on average, 282 cardiac calls daily, and 72% died.
As Lt. Michael Toomey, a 14-year veteran of the New York Fire Department notes, the number of patients in cardiac arrest appears to be quadrupling. Cardiac arrest is when the heart suddenly stops beating properly and cannot deliver blood to vital organs. These patients are clinically dead and will remain so unless they receive a defibrillation shock from an automated external defibrillator. Every minute that defibrillation is delayed, a patient’s survival chances decrease by 7-10%.
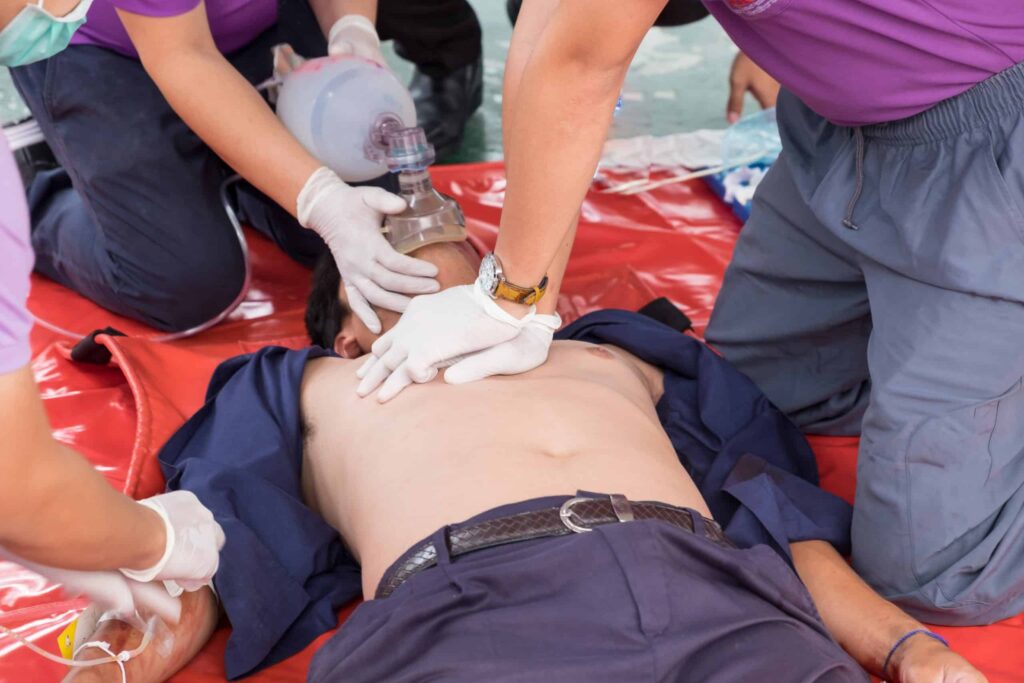
Additional Cardiac Arrest Risk Induced by COVID-19 Treatment
The risk of cardiac arrest among COVID-19 patients is also intensified by the possible side effects of quinolone the derives, hydroxychloroquine and chloroquine. These two drugs, primarily used to treat malaria, have been shown in limited studies to reduce viral load in COVID-19 patients.
Both drugs have received an Emergency Use Authorization from the Food and Drug Administration for COVID-19 treatment. While the promise of these drugs has been praised, there are complicating factors. Notably, both hydroxychloroquine and chloroquine are known to cause QT interval prolongation, a condition that predisposes patients to arrhythmias that cause sudden cardiac arrest. The American College of Cardiology has cautioned that both of these quinolone derivatives have the propensity to cause cardiac arrest. If patients take these drugs outside the hospital, without access to rapid defibrillation or regular heart monitoring with an ECG as recommended by the FDA, the risk of death intensifies.
EMS Protocols Change for Resuscitating Cardiac Arrest Patients

Coronavirus pathogenicity and the side effects of newly approved treatment options are not the only factors affecting cardiac arrest patients, emergency response, and survival. Hospitals are currently stretched beyond their limits, and as such, protocols for EMS response to out-of-hospital cardiac arrest are changing across the country.
The Regional Emergency Medical Services Council of New York has advised that, if a cardiac arrest patient cannot be revived in the field, the resuscitation should be terminated.
Typically, CPR and defibrillation are performed on cardiac arrest patients during ambulance transport to a nearby emergency room. However, CPR with rescue breaths is a high-risk procedure. The American Heart Association has accordingly released interim CPR guidelines that suggest not transporting cardiac arrest patients due to the low likelihood of survival balanced against the risk of COVID-19 exposure for pre-hospital and hospital providers. Hands-only or bystander CPR is still recommended for lay responders. Ultimately, as researchers from the New York-Presbyterian Hospital and Columbia Medical Center note, COVID-19 compromises the rapid triage of patients with cardiovascular conditions.
With the heart effects, treatment risks, and change in EMS protocols associated with COVID-19, considerable life may be lost due to cardiac arrest. This pandemic is devastating. Among many things, the threat of widespread sudden cardiac death speaks urgently to the need for affordable and accessible defibrillation.
Avive AED® Products for Sale
Shop Avive’s high-quality AED products, designed to empower communities to save lives.
Related Posts
In Pursuit of AED Incident Data: Nick Bogle’s Story
Nick Bogle’s Story I first have to say that my story has nothing to do with anything…
What Are the Common Causes of Cardiac Arrest in Infants and Children?
Discover the causes of cardiac arrest in children and infants and how to prevent this life-threatening condition...
Understanding First Aid Training & Its Importance
First aid training is designed to teach people the basic principles and techniques to provide immediate help…